
CHINESE JOURNAL OF PARASITOLOGY AND PARASITIC DISEASES ›› 2025, Vol. 43 ›› Issue (6): 806-813.doi: 10.12140/j.issn.1000-7423.2025.06.009
• ORIGINAL ARTICLES • Previous Articles Next Articles
HUANG Lihua( )(
)( ), LI Nan, GU Wei*(
), LI Nan, GU Wei*( )(
)( )
)
Received:2025-06-27
Revised:2025-09-20
Online:2025-12-30
Published:2025-12-29
Contact:
*E-mail:gw777@163.com
Supported by:CLC Number:
HUANG Lihua, LI Nan, GU Wei. Clinical characteristics of fascioliasis and primary liver cancer patients[J]. CHINESE JOURNAL OF PARASITOLOGY AND PARASITIC DISEASES, 2025, 43(6): 806-813.
Add to citation manager EndNote|Ris|BibTeX
URL: https://www.jsczz.cn/EN/10.12140/j.issn.1000-7423.2025.06.009
Table 1
Patients with fascioliasis in different cities (prefectures) have habits of ingesting contaminated food and/or drinking untreated water
| 市(州) Cities (prefectures) | 摄入组病例数(占比/%) Number of cases in the ingestion group (Proportion/%) | 未摄入组病例数(占比/%) Number of cases in the non-ingestion group (Proportion/%) |
|---|---|---|
| 昆明市 Kunming City | 2(2.0) | 1(1/9) |
| 大理白族自治州 Dali Bai Autonomous prefecture | 61(60.4) | 1(1/9) |
| 临沧市 Lincang City | 10(9.9) | 2(2/9) |
| 普洱市 Puer city | 11(10.9) | 2(2/9) |
| 楚雄彝族自治州 Chuxiong Yi Autonomous prefecture | 1(1.0) | 0(0) |
| 丽江市 Lijiang city | 13(12.9) | 2(2/9) |
| 保山市 Baoshan city | 2(2.0) | 1(1/9) |
| 昭通市 Zhaotong city | 1(1.0) | 0(0) |
Table 2
Comparison of characteristics between fasciolosisis and primary liver cancer patients
| 特征 Feature | 片形吸虫病(n = 110) Fasciolopsiasis(n = 110) | 原发性肝癌(n = 110) Primary liver cancer(n = 110) | 统计值 Statistic value | P值 P value |
|---|---|---|---|---|
| 年龄/岁 Age/year | 39.15 ± 15.05 | 57.85 ± 10.36 | t = 10.73 | < 0.01 |
| 脉搏/次·分-1 Pulse beats per minute | 91.58 ± 15.29 | 88.65 ± 13.32 | t = -1.51 | > 0.05 |
| 收缩压/mmHg Systolic blood pressure/mmHg | 118.43 ± 16.57 | 120.57 ± 17.67 | t = 0.93 | > 0.05 |
| 舒张压/mmHg Diastolic blood pressure/mmHg | 76.42 ± 10.37 | 76.98 ± 10.93 | t = 0.39 | > 0.05 |
| 住院时间/天 Hospitalization/d | 7.00(5.00, 10.75) | 8.00(5.00, 14.00) | Z = -0.75 | > 0.05 |
| 性别 Gender | ||||
| 男 Male | 44(40.0%) | 94(85.5%) | χ² = 48.60 | < 0.01 |
| 女 Female | 66(60.0%) | 16(14.6%) | ||
| 慢性乙型病毒性肝炎 Chronic viral hepatitis B | ||||
| 否No | 110(100%) | 9(8.2%) | χ² = 186.72 | < 0.01 |
| 是 Yes | 0(0) | 101(91.8%) | ||
| 慢性丙型病毒性肝炎 Chronic viral hepatitis C | ||||
| 否 No | 110(100%) | 108(98.2%) | χ² = 0.50 | > 0.05 |
| 是 Yes | 0(0) | 2(1.8%) | ||
| 慢性酒精性肝炎 Chronic alcoholic hepatitis | ||||
| 否 No | 110(100%) | 109(99.1%) | χ² = 1.00 | > 0.05 |
| 是 Yes | 0(0) | 1(0.9%) | ||
| 吸烟 Smoking | ||||
| 否 No | 93(84.5%) | 47(42.7%) | χ² = 41.56 | < 0.01 |
| 是 Yes | 17(15.5%) | 63(57.3%) | ||
| 饮酒 Alcohol consumption | ||||
| 否 No | 89(80.9%) | 58(52.7%) | χ² = 19.70 | < 0.01 |
| 是 Yes | 21(19.1%) | 52(47.3%) | ||
| 高血压 Hypertention | ||||
| 否 No | 100(90.9%) | 94(85.5%) | χ² = 1.57 | > 0.05 |
| 是 Yes | 10(9.1%) | 16(14.5%) | ||
| 糖尿病 Diabetes | ||||
| 否 No | 102(92.7%) | 100(90.9%) | χ² = 0.24 | > 0.05 |
| 是 Yes | 8(7.3%) | 10(9.1%) |
Table 3
Comparison of clinical manifestations between fascioliasis and primary liver cancer patients
| 临床表现 Clinical manifestation | 片形吸虫病病例数(占比/%) Number of fascioliasis cases (Proportion/%) | 原发性肝癌病例数(占比/%) Number of primary liver cancer cases (Proportion/%) | χ2值 χ2 value | P值 P value |
|---|---|---|---|---|
| 发热 Fever | 40(36.4) | 2(1.8) | 42.49 | < 0.01 |
| 腹痛 Abdominal pain | 41(37.3) | 71(64.6) | 16.37 | < 0.01 |
| 腹胀 Abdominal distention | 11(10.0) | 24(21.8) | 5.74 | < 0.05 |
| 乏力 Hypodynamina | 13(11.8) | 9(8.2) | 0.81 | > 0.05 |
| 纳差 Poor appetite | 7(6.4) | 6(5.5) | 0.08 | > 0.05 |
| 恶心 Nausea | 1(0.9) | 3(2.7) | 0.25 | > 0.05 |
| 厌油腻 Aversion to oil | 1(0.9) | 4(3.6) | 0.82 | > 0.05 |
| 体质量减轻 Weight loss | 2(1.8) | 18(16.4) | 14.08 | < 0.01 |
Table 4
Comparison of laboratory parameters between fasciolosisis and primary liver cancer patients
| 指标 Index | 片形吸虫病(n = 110)Fascioliasis (n = 110) | 原发性肝癌(n = 110)Primary liver cancer (n = 110) | 统计值 Statistic value | P 值 P value |
|---|---|---|---|---|
| 肿瘤标志物 Tumor marker | ||||
| 甲胎蛋白 Alpha-fetoprotein/ng·ml-1 | 3.31(2.31,5.35) | 400.00(16.26,1 210.00) | Z = -10.65 | < 0.01 |
| 癌胚抗原 Carcinoembryonic antigen/ng·ml-1 | 2.18(0.93,4.80) | 3.06(2.16,4.80) | Z = -3.03 | < 0.05 |
| 糖类抗原 Carbohydrate antigen 125/U·ml-1 | 14.40(9.71,18.17) | 41.89(19.18,222.90) | Z = -7.99 | < 0.01 |
| 糖类抗原 Carbohydrate antigen 153/U·ml-1 | 9.97(6.59,14.72) | 15.84(11.24,25.39) | Z = -6.05 | < 0.01 |
| 糖类抗原 Carbohydrate antigen 199/U·ml-1 | 14.03(5.08,19.26) | 26.66(14.65,70.98) | Z = -6.30 | < 0.01 |
| 凝血功能 Coagulation function | ||||
| 凝血酶原时间 Prothrombin time/s | 12.60(11.80,13.70) | 12.45(11.30,13.78) | Z = -0.50 | > 0.05 |
| 部分凝血酶原时间 Activated partial thromboplastin time/s | 31.84 ± 7.47 | 31.18 ± 6.37 | t = -0.70 | > 0.05 |
| 凝血酶时间 Thrombin time/s | 17.60(16.57,18.50) | 17.90(16.60,19.38) | Z = -1.36 | > 0.05 |
| 纤维蛋白原 Fibrinogen/g·L-1 | 3.35(2.79,4.41) | 3.06(2.40,3.89) | Z = -2.65 | < 0.05 |
| 血常规 Complete blood count | ||||
| 白细胞 White blood cell/ × 109·L-1 | 8.43(6.23,12.07) | 6.12(4.70,7.91) | Z = -5.63 | < 0.01 |
| 中性粒细胞百分比 Percentage of neutrophils/% | 38.30(30.13,46.85) | 65.25(56.42,72.80) | Z = -10.20 | < 0.01 |
| 嗜酸细胞百分比 Percentage of eosinophils/% | 29.15(16.40,38.18) | 1.65(0.70,3.08) | Z = -12.00 | < 0.01 |
| 嗜酸细胞绝对值 Absolute eosinophil count/ × 109·L-1 | 2.00(0.94,3.83) | 0.09(0.04,0.16) | Z = -12.05 | < 0.01 |
| 嗜酸细胞百分比 Percentage of eosinophils/% | χ2 = 138.70 | < 0.01 | ||
| 正常 Normal | 12(10.9%) | 80(72.7%) | ||
| 升高 Increase | 98(89.1%) | 11(10.0%) | ||
| 降低 Decrease | 0(0) | 19(17.3%) | ||
| 嗜酸细胞绝对值 Absolute eosinophil count/% | χ2 = 153.34 | < 0.01 | ||
| 正常 Norma | 18(16.4%) | 98(89.1%) | ||
| 升高 Increase | 92(83.6%) | 2(1.8%) | ||
| 降低 Decrease | 0(0) | 10(9.1%) | ||
| 红细胞 Red blood cell/ × 1012·L-1 | 4.50(3.98,4.80) | 4.31(3.73,4.99) | Z = -0.32 | > 0.05 |
| 血红蛋白 Hemoglobin/g·L-1 | 132.00(121.50,142.00) | 124.50(109.25,137.75) | Z = -2.76 | < 0.05 |
| 血小板 Platelet/ × 109·L-1 | 245.50(194.25,310.25) | 157.00(110.25,200.50) | Z = -7.75 | < 0.01 |
| 血生化 Blood biochemistry | ||||
| 总胆红素 Total bilirubin/µmol·L-1 | 9.25(7.03,12.40) | 17.35(11.98,30.68) | Z = -7.70 | < 0.01 |
| 直接胆红素 Direct bilirubin/µmol·L-1 | 3.50(2.70,4.70) | 6.80(4.70,16.35) | Z = -8.00 | < 0.01 |
| 间接胆红素 Indirect bilirubin/µmol·L-1 | 5.40(4.00,7.77) | 10.06(6.62,15.45) | Z = -6.69 | < 0.01 |
| 谷丙转氨酶 Alanine aminotransferase/U·L-1 | 24.00(17.00,48.00) | 46.50(27.00,68.50) | Z = -4.79 | < 0.01 |
| 谷草转氨酶 Aspartate aminotransferase/U·L-1 | 24.00(18.00,34.00) | 71.00(42.50,120.75) | Z = -9.02 | < 0.01 |
| 碱性磷酸酶 Alkaline phosphatase/U·L-1 | 143.00(98.00,190.50) | 150.00(111.00,221.75) | Z = -1.71 | > 0.05 |
| 总蛋白 Total protein/g·L-1 | 69.80(66.12,75.45) | 67.75(62.08,72.20) | Z = -3.46 | < 0.01 |
| 白蛋白 Albumin/g·L-1 | 36.10(32.92,38.98) | 33.75(29.60,37.65) | Z = -2.81 | < 0.05 |
| 球蛋白 Globulin/g·L-1 | 33.05(28.52,40.55) | 32.35(28.30,36.38) | Z = -1.69 | > 0.05 |
| γ-谷氨酰转肽酶 Gamma-glutamyl transpeptidase/U·L-1 | 74.00(44.25,124.50) | 138.00(73.00,267.50) | Z = -4.91 | < 0.01 |
| 尿素 Urea/mmol·L-1 | 4.56(3.64,5.50) | 4.68(3.92,5.60) | Z = -1.06 | > 0.05 |
| 肌酐 Creatinine/µmol·L-1 | 64.00(55.55,75.00) | 67.00(57.00,74.00) | Z = -0.62 | > 0.05 |
| 尿酸 Uric acid/µmol·L-1 | 313.22 ± 80.98 | 331.15 ± 96.23 | t = 1.50 | > 0.05 |
| 血钾 Serum potassium/mmol·L-1 | 3.91 ± 0.41 | 3.99 ± 0.40 | t = 1.48 | > 0.05 |
| 血钠 Serum sodium/mmol·L-1 | 140.00(138.00,142.00) | 139.00(138.00,142.00) | Z = -1.60 | > 0.05 |
| 血氯 Serum chloride/mmol·L-1 | 104.40(103.12,106.52) | 104.30(101.15,106.18) | Z = -1.41 | > 0.05 |
| 血钙 Serum calcium/mmol·L-1 | 2.22(2.13,2.32) | 2.24(2.13,2.32) | Z = -0.36 | > 0.05 |
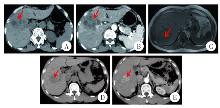
Fig. 1
Comparison of abdominal imaging features between fasciolosisis (A, B, C) and primary liver cancer (D, E) patients A: In the venous phase of abdominal CT, multiple quasi-circular hypodense lesions are visible in the right hepatic lobe, distributed in a clustered pattern; B: In the arterial phase of abdominal CT, hepatic lesions demonstrate no significant enhancement; C: In abdominal magnetic resonance imaging, hepatic segments 6 and 7 demonstrate patchy hypointense lesions; D: In the venous phase of abdominal CT, nodular hypodense lesions are observed in the right hepatic lobe; E: In the arterial phase of abdominal CT, significant enhancement is observed within the lesions in the right hepatic lobe.
|
| [1] | CHEN Chong, ZHU Aihong, HUANG Qin. Current status and research progress of triclabendazole resistance in fascioliasis treatment [J]. CHINESE JOURNAL OF PARASITOLOGY AND PARASITIC DISEASES, 2025, 43(5): 718-722. |
| [2] | YAN Dongning, ZHANG Keru, LI Changling, CHEN Xiaojun. Clinical and epidemiologic features of visceral leishmaniasis: A retrospective analysis of 49 cases [J]. CHINESE JOURNAL OF PARASITOLOGY AND PARASITIC DISEASES, 2025, 43(4): 547-554. |
| [3] | CHENG Li, YANG Chengming, ZHANG Ni, XU Xiaonan, LI Yuanxiao, LI Yan, MA Hanwei, LIU Hui, DAI Xingxing. Clinical features and diagnosis and treatment effect in 47 children cases of visceral leishmaniasis in Gansu Province [J]. CHINESE JOURNAL OF PARASITOLOGY AND PARASITIC DISEASES, 2023, 41(6): 772-775. |
| [4] | LI Xiaoli, LI Shaogang, WU Zhaoyong. Clinical characteristics of patients with intestinal Diphyllobothrium tapeworm infection [J]. CHINESE JOURNAL OF PARASITOLOGY AND PARASITIC DISEASES, 2023, 41(4): 459-463. |
| [5] | Wei-na ZHANG, Wei GU, Jian-ming JIAO, Jiao LUO. Analysis of clinical features on 15 case of fascioliasis [J]. CHINESE JOURNAL OF PARASITOLOGY AND PARASITIC DISEASES, 2019, 37(2): 207-212. |
| [6] | Yan ZHOU, Yan-hong XIONG, Xue-nian XU. Interpretation of the Criteria for Diagnosis of Fascioliasis [J]. CHINESE JOURNAL OF PARASITOLOGY AND PARASITIC DISEASES, 2018, 36(4): 425-428. |
| [7] | CHEN Feng1,YANG Hui1,LIU Yu-hua1 *,DUAN Yu-chun1,YANG Jing1,CUI Yu-hua1,YANG Li-qun1,YANG Qiong1,ZHANG Jian-guo2,LUO Jia-jun1. Epidemiological Investigation of Fascioliasis and Analysis of a Chronic Human Fascioliasis Case in Binchuan County,Yunnan Province [J]. , 2014, 32(6): 17-422-424. |
| [8] | LIU Qian, CHENG Na, ZHOU Yan, XU Xue-nian*. Research Progress on Fascioliasis [J]. , 2013, 31(3): 15-229-234. |
| Viewed | ||||||
|
Full text |
|
|||||
|
Abstract |
|
|||||